
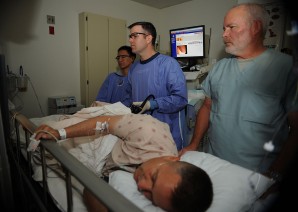
An endoscope is inserted in the patients rectum and pushed up through his bowels during a colonoscopy procedure. Cleaning the endoscopes after each use is a huge problem, doctors don’t like to discuss.
Recently l have been doing research into procedures currently used for cleaning flexible fiber optic endoscopes. Many people are unaware that flexible endoscopes aren’t by design very infection control friendly.
Endoscopes are commonly used in colonoscopy procedures.
In fact cleaning endoscopes thoroughly is next to impossible.
Part of the problem is that the devices contain internal air and water channels too small to insert brushes all the way through to clean out, feces, blood and tissue debris.
The other problem is disinfection techniques currently used are simply inadequate to deal with the problem. I found sterilization is better than disinfection but still doesn’t kill spores. In most cases endoscopic specialists adopt disinfection as the preferred method.
I also discovered that flushing is better than soaking in disinfectant and germicide. For example doubling your flow rate doubles the chance that disinfection can attack the bio-films, blood particles and feces and other patient materials lodged in minute crannies of endoscopes.
In most cases endoscopy clinics use machines to circulate germicidal solutions over the internal/external parts and surfaces, but only soak them on average of ten minutes, according to my source at St. Joseph’s Hospital in Phoenix, Arizona. When it would take hours of soaking to reach acceptable sterilization conditions.
The sad fact is only one in ten endoscopy units at major hospitals follow current FDA requirements for properly cleaning, disinfecting and sterilization of endoscopes. And in those cases where they do only a little more than half reprocess flexible endoscopes properly, in terms of following cleaning/ disinfecting steps that conform to infection control guidelines.
See related articles: Preventing Cross-Contamination in Endoscope Processing: FDA Safety Communication http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm190273.htm
Even in those rare cases where practitioners try their best and say switch from soaking and flushing endoscopes in glutaraldehyde to purging devices with buffered peracetic acid have experienced an initial increase in repairs of those devices.
One lab tech I convinced to run some tests indicated that the use of peracetic acid exposes minute micro cracks and internal channels. Saying many endoscopes are held together by potentially infectious patient material he called “superbio glue” containing microorganisms buried under layers of glutaraldehyde hardened surfaces. Which is freaking gross!
Needless to say recommended guidelines for reprocessing endoscopes should be upgrades from high level disinfection to employment of sterile disposable sleeves and (stealth) shields which are years away from development…
Whats needed I think is a radical redesign of the endoscope device, but I lack the technical and engineering expertise to develop.
See also: Guideline for Disinfection and Sterilization in Healthcare Facilities, 2008http://www.cdc.gov/hicpac/disinfection_sterilization/3_0disinfectequipment.html

